Balance is something most people rarely think about until it starts becoming more difficult.
But as we age, gradual physical changes can affect coordination, posture, walking ability, and overall stability.
Many older adults notice they feel less steady while walking, turning quickly, climbing stairs, or getting up from a chair – and this is usually the result of these gradual changes.
While some decline in balance is a normal part of aging, frequent unsteadiness or falls should never be ignored.
Understanding why balance changes occur can help seniors take steps to improve stability, reduce fall risk, and maintain independence.
Why Balance Changes With Age
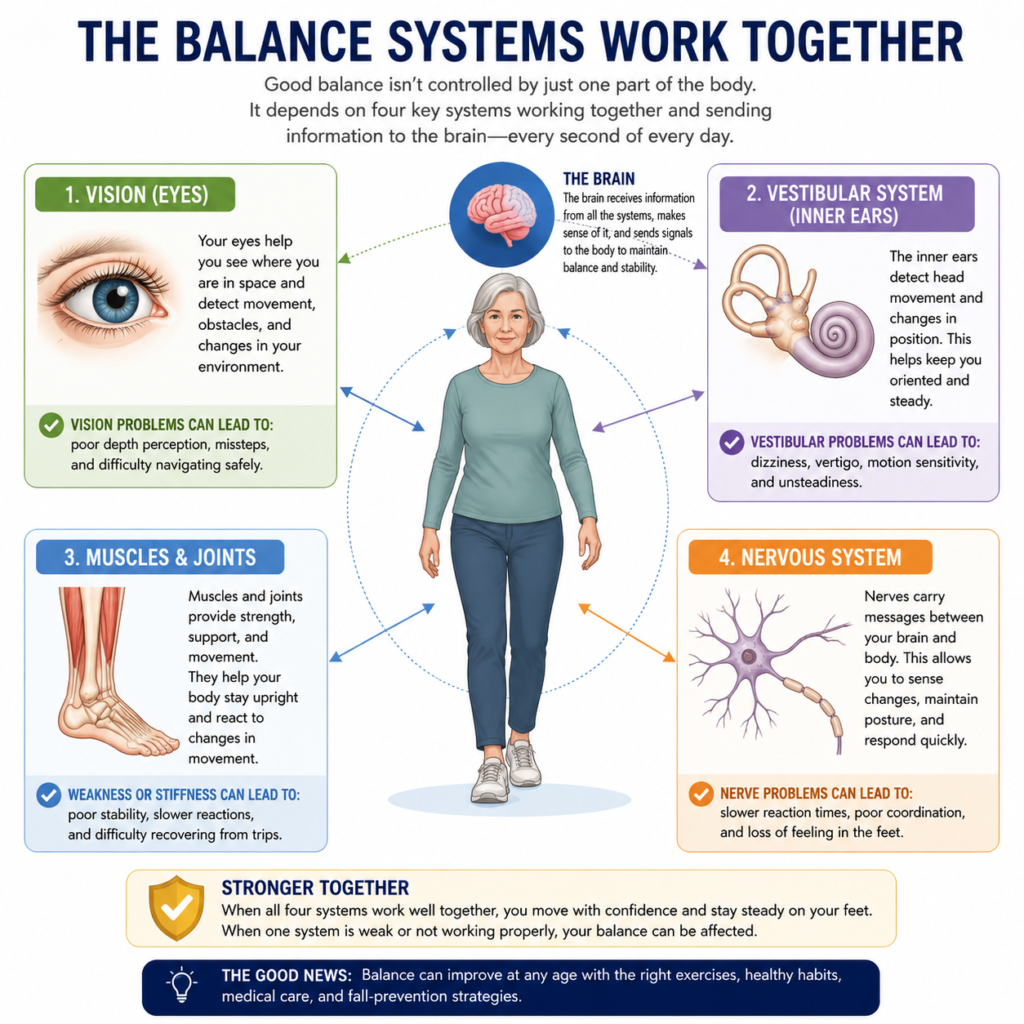
Balance depends on several body systems working together continuously.
The brain constantly processes information from the eyes, inner ears, muscles, joints, and nervous system to keep the body upright and stable.
As people grow older, these systems gradually become less efficient and even mild decline across multiple areas can noticeably affect balance and coordination.
Muscle Loss and Weakness
One of the biggest contributors to poor balance in older adults is age-related muscle loss, known as sarcopenia.
Beginning around age 30, adults gradually lose muscle mass over time, and this process often accelerates after age 60.
Weakness in the legs and core muscles makes it harder to stabilize the body, recover from trips, and safely perform daily activities.
The muscles surrounding the hips and ankles are especially important for balance control.
When these muscles weaken, older adults may struggle to react quickly enough to sudden instability or uneven surfaces.
Reduced muscle power also affects reaction time, making falls more likely after stumbling.
Slower Reflexes and Nervous System Changes
The nervous system naturally slows with age.
Communication between the brain and muscles may become less efficient, delaying the body’s ability to respond to sudden movement or balance disturbances.
In younger adults, balance corrections often occur almost instantly. In seniors though, these protective responses may take longer, increasing the risk of losing stability after slips or trips.
This slower reaction time becomes especially noticeable when walking on uneven ground, changing direction quickly, or navigating crowded environments.
Vision Changes and Balance
Vision plays a major role in maintaining balance and spatial awareness.
As humans, most of us are quite dependent on our eyes for continuously telling the brain info regarding our body position.
And as people age, vision commonly becomes less sharp and less adaptable in low-light conditions.
Depth perception, peripheral vision, and contrast sensitivity may also decline.
Common eye conditions such as cataracts, glaucoma, and macular degeneration can further impair balance and increase fall risk.
Poor vision makes it harder to judge distances, detect obstacles, and safely navigate stairs or uneven surfaces.
Inner Ear Changes
The inner ear contains the vestibular system, which helps detect movement and maintain equilibrium.
Over time, the sensory structures within the inner ear become less sensitive. This may reduce the brain’s ability to accurately detect changes in body position and movement.
As vestibular function declines, seniors may experience dizziness, vertigo, motion sensitivity, or unsteadiness while walking.
These changes are one reason older adults often feel less stable when turning quickly or moving through busy environments.
Reduced Sensation in the Feet and Legs
The brain relies heavily on feedback from the feet and legs to maintain stability.
Nerves continuously send information about pressure, movement, and body position and the body depends on these signals for maintaining balance.
Conditions such as peripheral neuropathy can reduce sensation in the lower extremities, making it harder to detect uneven surfaces or properly sense foot placement.
Without accurate sensory feedback, balance becomes less reliable – especially in dim lighting or on unstable ground.
Numbness, tingling, or reduced sensation in the feet significantly increases fall risk in older adults.
Joint Stiffness and Reduced Mobility
Arthritis and age-related joint stiffness can also interfere with balance and walking mechanics.
Reduced mobility in the ankles, knees, hips, or spine may limit the body’s ability to make rapid balance adjustments.
Pain frequently changes walking patterns as well, causing many seniors to take shorter steps or move more cautiously.
Although these adaptations may temporarily improve confidence, they can sometimes reduce walking efficiency and contribute to long-term instability.
Blood Pressure and Circulation Changes
Aging affects the cardiovascular system in several ways.
Blood vessels gradually become less flexible, and the body may become slower at regulating blood pressure during movement or position changes.
Some older adults experience dizziness or lightheadedness when standing up due to temporary drops in blood pressure, known as orthostatic hypotension.
Reduced blood flow to the brain can briefly impair balance and increase the likelihood of falls.
Dehydration, medications, and heart conditions may worsen these symptoms.
Medication Effects on Balance
Many medications commonly prescribed to seniors can affect alertness, coordination, blood pressure, or reaction time.
Blood pressure medications, sedatives, antidepressants, sleep aids, and certain pain medications are common contributors to balance problems and dizziness.
In some cases, instability is related more to medication side effects or interactions than aging itself.
Why Balance Problems Increase Fall Risk
Balance decline becomes dangerous because even brief episodes of instability can lead to serious injury.
Falls are one of the leading causes of hospitalization, fractures, and loss of independence in older adults.
As a home health physical therapist, I see a lot of patients that have had one or more falls and a big goal is always to improve balance and try to figure out ways to reduce fall risk.
Fear of falling may also cause seniors to become less active, which can further weaken muscles and worsen balance over time.
This often creates a cycle where inactivity contributes to increasing weakness and instability.
Common Age-Related Changes That Affect Balance
Several normal age-related changes can gradually affect balance, coordination, and walking stability in older adults.
| Age-Related Change | How It Affects Balance |
|---|---|
| Muscle weakness | Reduces stability and ability to recover from trips |
| Slower reflexes | Delays balance corrections during movement |
| Vision decline | Makes obstacles and uneven surfaces harder to detect |
| Inner ear changes | Affects spatial orientation and equilibrium |
| Reduced foot sensation | Makes foot placement less accurate |
| Joint stiffness | Limits movement and balance adjustments |
| Blood pressure fluctuations | Can cause dizziness or faintness |
| Medication side effects | May impair coordination or alertness |
In many seniors, balance decline is caused by several of these factors occurring at the same time rather than a single issue alone.
Signs of Balance Problems in Older Adults
Balance decline often develops gradually. Seniors may notice increasing difficulty walking safely, turning quickly, or navigating uneven surfaces.
Common warning signs of balance loss include:
- shuffling while walking
- needing support for stability
- dizziness when standing
- difficulty climbing stairs
- bumping into objects
- fear of falling
- feeling unsteady in crowds
Persistent balance problems or repeated falls should always be evaluated by a healthcare professional.
Can Balance Improve With Age?
Yes!
Although some age-related changes cannot be completely reversed, balance can often improve significantly with proper treatment and exercise.
Research consistently shows that physical activity helps improve strength, coordination, walking ability, reaction time, and confidence in older adults.
I always tell my patients though, that improving balance takes time – often more time than improving strength does.
A lot will depend on the underlying causes of the balance issues, but it’s important to understand that consistency is key.
Addressing contributing factors such as poor vision, dehydration, medication side effects, and foot pain may also improve overall stability as well.
How Seniors Can Improve Balance and Stability
Several lifestyle changes and preventive strategies may help reduce balance decline and lower fall risk.
Regular exercise is one of the most effective interventions and this is where physical therapy really comes in.
Walking, strength training, tai chi, and balance-focused exercises can improve muscle strength, coordination, and posture control.
Maintaining good vision through regular eye exams, wearing supportive footwear, reviewing medications regularly, and improving home safety can also help reduce falls.
Simple home modifications such as better lighting, grab bars, and removing loose rugs may significantly improve safety for seniors with balance concerns.
Final Thoughts
Balance and stability rely on many body systems working together efficiently.
And as we age, gradual changes in muscle strength, reflexes, vision, circulation, joint mobility, and inner ear function can all contribute to unsteadiness.
Although some decline is common with aging, serious balance problems should never be considered inevitable.
With regular physical activity, medical management, and fall prevention strategies, many seniors can improve stability, remain active, and maintain independence well into later life.
Frequently Asked Questions
Is poor balance a normal part of aging?
Some balance decline is common with aging, but severe instability or repeated falls are not considered normal and should be evaluated.
Why do seniors become unsteady while walking?
Balance problems often result from a combination of muscle weakness, slower reflexes, vision decline, inner ear changes, and reduced sensation in the feet.
Can exercise improve balance in older adults?
Yes! Strength and balance exercises can significantly improve stability and reduce fall risk.
What medical conditions affect balance in seniors?
Conditions such as arthritis, diabetes, neuropathy, Parkinson’s disease, stroke, and inner ear disorders may all contribute to balance problems.
When should balance problems be evaluated?
Balance issues should be evaluated if they are worsening, causing falls, limiting activity, or accompanied by dizziness or weakness.



